 The highest pain score recorded in the PACU was 4 (0–10) for the PRE group and 1 (0–9) for the POST group (P = 0.597). The lowest pain score recorded in the PACU was 0 (0–5) for the PRE group and 0 (0–4) for the POST group (P = 0.444). Sixteen PRE patients (50%) and 26 POST patients (54%) required no opioids in the PACU (P = 0.715). In the PACU, overall opioid consumption in MME (median ) was 4 (0–65) for the PRE group and 0 (0–62) for the POST group (P = 0.584). Other outcomes included opioid consumption per POD in morphine mg equivalents (MME) with POD 0 including PACU stay lowest and highest pain scores on POD 1 and 2 length of stay discharge disposition maximum ambulation distance on POD 1 and 2 and 30-day adverse events such as new peripheral neuropathies, emergency room visits, hospital readmissions, and major organ system complications. Daily pain scores were broken down into the lowest reported pain score and the highest reported pain score. Pain was assessed at least once every 4 h per nursing protocol as well as before and after each as-needed analgesic administration. POD 0 data included PACU and ward measures on the surgical date the number of ward measures varied depending on the time of admission to the ward. Since LIA is only expected to last approximately 12 h, the primary outcome for this study was patient-reported pain scores (numeric rating scale 0 = no pain 10 = worst possible pain) on POD 0. Baseline characteristics included: age, sex, height, weight, body mass index, American Society of Anesthesiologists physical status, pre-operative opioid prescription (any active opioid prescription within the previous year), case length (out-of-room time minus inroom time), and anesthesia type. Data normally collected during the postoperative course related to pain, medication administration, and rehabilitation were included and retrospectively reviewed. Twenty ml of 0.2% ropivacaine was injected incrementally into this space.ĭata were collected for consecutive TKA patients 4 months post-IPACK implementation (POST) and compared to those for a historical cohort comprised of consecutive TKA patients by the same surgeon 4 months prior to IPACK implementation (PRE). Using an in-plane approach, an 8.9 cm 20-gauge Tuohy-tip needle (Epimed, USA) was inserted from medial to lateral to position the needle tip between the popliteal artery and the femur ( Fig. 
If the femoral condyles were seen, the transducer was moved proximally to a position over the distal femoral shaft. 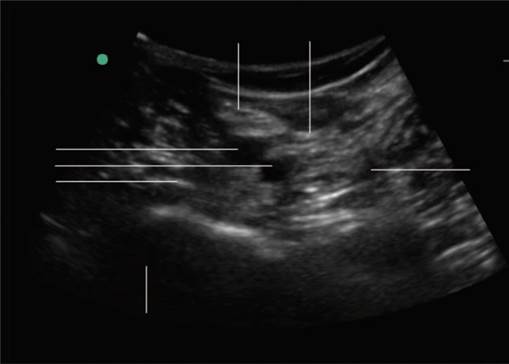
A high-frequency ultrasound transducer (HFL50, FUJIFILM Sonosite, USA) was used to visualize the popliteal artery and posterior surface of the distal femur ( Fig. Sanjay Sinha (personal communication), the leg was positioned with the knee flexed and hip externally rotated. In the IPACK implementation cohort, after the ACC insertion, the IPACK block was performed under ultrasound guidance using a sterile technique with the operative extremity cleansed from the inguinal ligament down to the popliteal crease. All other TKA patients continued to receive surgeon-administered LIA.įor all patients undergoing knee arthroplasty surgery, the RAAPM team placed an ultrasound-guided adductor canal catheter (ACC) pre-operatively using a technique described previously. 
The IPACK technique was researched and disseminated to RAAPM team members, and the project was initiated in May 2018 for all knee arthroplasty patients of this single surgeon. 
A collective decision was made for the RAAPM team to provide pre-operative IPACK blocks as part of the TKA clinical pathway with strong support from the new surgeon who favored this approach due to the timing (prior to insertion of implants) and image guidance (ultrasound). A need for an infiltrative technique was identified and options included LIA administered by the new surgeon or IPACK blocks performed by the RAAPM team. The steps were planned in advance with various stakeholder groups including RAAPM anesthesiologists, orthopedic surgeons, and nurses in the post-anesthesia care unit (PACU) and surgical ward. This implementation of a clinical practice change was designed as a quality improvement project using 1 cycle of a plan-do-study-act. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
